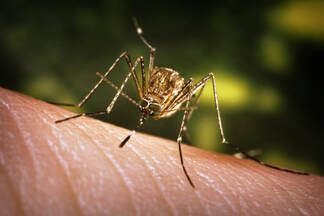
 Japanese Encephalitis mosquito Culex Tritaeniorhynchus - Image Credit: WHO
Japanese Encephalitis mosquito Culex Tritaeniorhynchus - Image Credit: WHO
Japanese encephalitis is a viral disease that primarily affects the brain and is transmitted by mosquitoes. It is a serious health concern in many parts of Asia, particularly in rural areas where farming and rice cultivation are prevalent.
Get a comprehensive overview of Japanese encephalitis, including its causes, symptoms, treatment options, and preventive measures.
Get a comprehensive overview of Japanese encephalitis, including its causes, symptoms, treatment options, and preventive measures.
What is Japanese Encephalitis?
A viral disease, Japanese encephalitis (JE) is caused by the Japanese encephalitis virus (JEV), a member of the Flavivirus genus. It is primarily transmitted through the bite of infected Culex mosquitoes, which breed in rice fields and waterlogged areas. The virus primarily affects the central nervous system, leading to inflammation of the brain (encephalitis).
How common is Japanese Encephalitis?
The exact prevalence of Japanese encephalitis can vary from year to year and by geographic location. According to the World Health Organization (WHO), an estimated 68,000 cases of Japanese encephalitis occur worldwide every year. According to estimates, the incidence of Japanese encephalitis among travelers is less than 1 in a million in any given year.
However, it is important to note that these figures may be an underestimate due to under-reporting and misdiagnosis in regions with limited healthcare access.
Vaccination plays a crucial role in preventing Japanese encephalitis. The WHO recommends routine immunization as part of national immunization programs in areas where the disease is endemic. The disease is endemic in many parts of Asia, including rural and agricultural areas, and it can result in severe neurological complications, including inflammation of the brain.
The highest burden of Japanese encephalitis is observed in countries such as China, India, and other Southeast Asian nations. These regions experience regular outbreaks, particularly during the rainy season when mosquito populations are higher. However, sporadic cases or localized outbreaks have also been reported in other parts of Asia, the Pacific Islands, and even in some parts of Australia.
It is essential to consult healthcare professionals or relevant authorities for the most accurate and specific information regarding Japanese encephalitis in your particular region or if you have any concerns about the disease.
However, it is important to note that these figures may be an underestimate due to under-reporting and misdiagnosis in regions with limited healthcare access.
Vaccination plays a crucial role in preventing Japanese encephalitis. The WHO recommends routine immunization as part of national immunization programs in areas where the disease is endemic. The disease is endemic in many parts of Asia, including rural and agricultural areas, and it can result in severe neurological complications, including inflammation of the brain.
The highest burden of Japanese encephalitis is observed in countries such as China, India, and other Southeast Asian nations. These regions experience regular outbreaks, particularly during the rainy season when mosquito populations are higher. However, sporadic cases or localized outbreaks have also been reported in other parts of Asia, the Pacific Islands, and even in some parts of Australia.
It is essential to consult healthcare professionals or relevant authorities for the most accurate and specific information regarding Japanese encephalitis in your particular region or if you have any concerns about the disease.
Japanese Encephalitis Causes: Why and How Does Japanese Encephalitis Spread?
Japanese encephalitis (JE) is a viral infection that primarily affects the central nervous system. It is caused by the Japanese encephalitis virus (JEV), which is transmitted to humans through the bite of infected mosquitoes. Understanding how Japanese encephalitis spreads is crucial for implementing effective prevention and control strategies. Explore the transmission cycle of Japanese encephalitis and the factors contributing to its spread.
1. Mosquito Vector
Japanese encephalitis is primarily transmitted by mosquitoes, particularly those belonging to the Culex species, with Culex tritaeniorhynchus being the primary vector. These mosquitoes typically breed in flooded rice fields and other stagnant water sources, and they are most active during the evening and night. Infected mosquitoes acquire the Japanese encephalitis virus by feeding on infected vertebrate hosts, such as pigs and water birds.
2. Amplifying Hosts
Pigs play a significant role in the transmission cycle of Japanese encephalitis. They act as amplifying hosts, as the virus can replicate within their bloodstream, leading to high levels of virus circulation. Infected pigs do not develop severe symptoms but serve as a reservoir for the virus. Mosquitoes that feed on infected pigs become infected themselves and can transmit the virus to other animals or humans.
3. Transmission to Humans
When a mosquito carrying the Japanese encephalitis virus bites a human, the virus can be transmitted and cause infection. Humans are considered incidental or dead-end hosts because the virus does not reach high levels in their bloodstream. However, some individuals may develop symptoms of Japanese encephalitis, which can range from mild flu-like illness to severe neurological complications, including inflammation of the brain (encephalitis).
4. Geographical Distribution
Japanese encephalitis is prevalent in many parts of Asia and the Western Pacific region. It is endemic in rural and agricultural areas where the mosquito vector and amplifying hosts, such as pigs and water birds, are abundant. Countries with high incidence include China, Japan, South Korea, Vietnam, Thailand, and India.
Culex tritaeniorhynchus, the Japanese Mosquito
Culex tritaeniorhynchus is a species of mosquito commonly known as the Oriental mosquito or Japanese encephalitis mosquito. It belongs to the family Culicidae and is considered a significant vector for transmitting the Japanese encephalitis virus (JEV) among humans and animals. These mosquitoes are primarily found in rural and agricultural areas, particularly in regions of Southeast Asia and the Western Pacific where Japanese encephalitis is endemic.
Culex tritaeniorhynchus mosquitoes typically breed in rice fields and irrigated agricultural areas, and their bites can transmit the JEV, which causes Japanese encephalitis in humans. Preventive measures, including mosquito control and vaccination, are essential in areas where Culex tritaeniorhynchus mosquitoes are prevalent to reduce the risk of Japanese encephalitis transmission.
Culex tritaeniorhynchus mosquitoes typically breed in rice fields and irrigated agricultural areas, and their bites can transmit the JEV, which causes Japanese encephalitis in humans. Preventive measures, including mosquito control and vaccination, are essential in areas where Culex tritaeniorhynchus mosquitoes are prevalent to reduce the risk of Japanese encephalitis transmission.
Japanese Encephalitis Symptoms
Symptoms of Japanese encephalitis can vary from mild to severe and can appear 5 to 15 days after the mosquito bite. In most cases, individuals infected with the virus do not develop any symptoms. However, when symptoms do occur, they can range from a mild flu-like symptom to severe neurological complications. Here are some of the common symptoms associated with Japanese encephalitis:
- Fever: Fever is often the initial symptom and can range from low-grade to high-grade.
- Headache: Persistent and severe headaches are common symptoms of JE. The headache may be accompanied by sensitivity to light (photophobia).
- Stiff neck: Neck stiffness is a classic symptom of meningitis, which can occur in severe cases of Japanese encephalitis.
- Nausea and vomiting: Some individuals may experience gastrointestinal symptoms such as nausea and vomiting.
- Fatigue and weakness: Generalized weakness and fatigue are common, especially in the early stages of the disease.
- Altered mental state: As the disease progresses, individuals may experience confusion, irritability, and changes in behavior.
- Seizures: Seizures can occur in severe cases of Japanese encephalitis.
- Muscle weakness or paralysis: In some cases, muscle weakness or paralysis, particularly in the limbs, may be observed.
- Tremors and involuntary movements: Individuals may experience tremors, muscle twitching, or other involuntary movements.
- Coma: In severe cases, Japanese encephalitis can lead to a state of coma.
When to Seek Medical Attention for Japanese Encephalitis?
It is important to note that not all individuals infected with the Japanese encephalitis virus will develop symptoms, and the severity of symptoms can vary widely. However, in cases where symptoms are present, especially neurological symptoms, immediate medical attention should be sought.
Japanese Encephalitis Diagnosis
If you suspect that you or someone you know may have Japanese encephalitis, it is important to consult a healthcare professional for a proper diagnosis. Laboratory tests, such as blood tests and cerebrospinal fluid analysis, can help confirm the presence of the virus.
Diagnosing Japanese encephalitis requires laboratory tests to detect the presence of the virus in blood or cerebrospinal fluid.
Diagnosing Japanese encephalitis requires laboratory tests to detect the presence of the virus in blood or cerebrospinal fluid.
Japanese Encephalitis Prevention
Prevention and control measures for Japanese encephalitis primarily focus on reducing mosquito populations, protecting individuals from mosquito bites, and vaccinating susceptible populations. Vaccination campaigns targeting high-risk areas and age groups have been effective in reducing the burden of Japanese encephalitis in several countries.
Japanese Encephalitis Treatment
There is no specific antiviral treatment for JE, and management focuses on supportive care to alleviate symptoms and reduce complications. Hospitalization may be necessary for severe cases.
1. Supportive Care:
- Hospitalization: Severe cases of Japanese encephalitis may require hospitalization for close monitoring and intensive care.
- Rest and hydration: Patients are advised to get plenty of rest and drink an adequate amount of fluids to prevent dehydration.
- Fever management: Antipyretic medications like acetaminophen can be used to manage fever and discomfort.
- Seizure control: Anticonvulsant medications may be prescribed to control seizures if they occur.
- Respiratory support: In severe cases with respiratory distress, mechanical ventilation may be necessary.
2. Symptom Management
- Pain relief: Analgesics may be prescribed to alleviate headaches and body aches.
- Antiemetics: Medications to control nausea and vomiting can be administered.
- Anti-inflammatory drugs: Nonsteroidal anti-inflammatory drugs (NSAIDs) may help reduce inflammation and relieve symptoms.
- Anticonvulsants: If seizures occur, anticonvulsant medications can be used to manage them.
3. Prevention of Complications
- Intracranial pressure management: In cases where increased pressure inside the skull is observed, measures to control and reduce intracranial pressure may be necessary.
- Fluid and electrolyte balance: Maintaining proper hydration and electrolyte balance is crucial to prevent complications.
- Nutrition support: Adequate nutrition should be provided to support the body's immune response and recovery.
- Rehabilitation: Physical therapy, occupational therapy, and speech therapy may be required to aid in the recovery of motor skills, coordination, and speech abilities.
Vaccination is an effective preventive measure against Japanese encephalitis. The JE vaccine is recommended for individuals traveling to or residing in areas with a high risk of JE transmission.
It is essential to take preventive measures to avoid mosquito bites, such as using mosquito repellents, wearing protective clothing, and sleeping in screened or air-conditioned rooms. Vector control programs, including mosquito eradication and vaccination campaigns, are also implemented in high-risk areas to reduce the spread of Japanese encephalitis.
Remember to consult a healthcare professional or travel health clinic for personalized advice and guidance regarding Japanese encephalitis prevention and treatment.
Japanese Encephalitis Risk Factors and Geographical Distribution
Japanese encephalitis is most common in rural agricultural areas, where humans live in close proximity to domestic pigs and water birds, which serve as amplifying hosts for the virus. The disease is prevalent in parts of Asia, including Southeast Asia, India, China, Japan, and some Pacific islands.
Japanese Encephalitis Vaccination
Vaccination is a crucial preventive measure against Japanese encephalitis. The World Health Organization (WHO) recommends JE vaccine for individuals residing in or traveling to endemic areas. Vaccination campaigns targeting children have significantly reduced the burden of the disease in many countries.
Other preventive measures include mosquito control strategies such as using bed nets, insect repellents, and minimizing exposure during peak mosquito activity hours. Additionally, personal protective measures such as wearing long-sleeved clothing can help reduce the risk of mosquito bites.
The Japanese encephalitis vaccine is generally given in a series of two doses, with booster doses recommended for long-term protection. It is important to consult with a healthcare professional for advice on vaccination and the recommended schedule. The vaccine is highly effective and provides long-term protection.
JE vaccine helps protect individuals, particularly those residing in or traveling to high-risk areas, from contracting the disease. Vaccination also contributes to reducing the overall burden of Japanese Encephalitis in endemic regions and curbing the spread of the virus.
There are several vaccines available, including inactivated and live attenuated vaccines. These vaccines stimulate the immune system to produce protective antibodies against the Japanese Encephalitis virus, providing immunity.
Other preventive measures include mosquito control strategies such as using bed nets, insect repellents, and minimizing exposure during peak mosquito activity hours. Additionally, personal protective measures such as wearing long-sleeved clothing can help reduce the risk of mosquito bites.
The Japanese encephalitis vaccine is generally given in a series of two doses, with booster doses recommended for long-term protection. It is important to consult with a healthcare professional for advice on vaccination and the recommended schedule. The vaccine is highly effective and provides long-term protection.
JE vaccine helps protect individuals, particularly those residing in or traveling to high-risk areas, from contracting the disease. Vaccination also contributes to reducing the overall burden of Japanese Encephalitis in endemic regions and curbing the spread of the virus.
There are several vaccines available, including inactivated and live attenuated vaccines. These vaccines stimulate the immune system to produce protective antibodies against the Japanese Encephalitis virus, providing immunity.
Japanese Encephalitis Vaccine Administration
The Japanese Encephalitis vaccine is administered through an intramuscular injection. The number of doses and the JE vaccine schedule may vary depending on the vaccine used. It is important to follow the recommended dosage and schedule for optimal protection.
Japanese Encephalitis Vaccine Effectiveness
Studies have shown that the Japanese Encephalitis vaccine is highly effective in preventing the disease. It provides long-term immunity, reducing the risk of infection and severe complications. However, like any vaccine, its effectiveness may vary among individuals.
Japanese Encephalitis Vaccine Side Effects
The Japanese Encephalitis vaccine is generally safe and well-tolerated. Common side effects of the JEV vaccine include mild pain, redness, or swelling at the injection site. Rarely, individuals may experience fever, headache, or muscle aches. Serious adverse reactions are extremely rare.
Who Should Get Vaccinated with the JE Vaccine?
Individuals living in or traveling to areas with a high risk of Japanese Encephalitis should consider vaccination. This includes travelers visiting rural areas, agricultural workers, and individuals involved in outdoor activities during the transmission season. Consultation with a healthcare professional or travel medicine specialist is advised to assess the need for a JEV vaccine based on individual circumstances.
Japanese Encephalitis Vaccine Precautions and Recommendations
- The Japanese Encephalitis vaccine is generally safe for most individuals, but it may not be suitable for those with certain medical conditions. Consultation with a healthcare professional is essential to evaluate the appropriateness of vaccination.
- It is important to continue taking preventive measures against mosquito bites, such as using insect repellents, wearing protective clothing, and staying in screened or air-conditioned accommodations.
- JEV vaccine should be administered at least a few weeks before traveling to allow sufficient time for the immune response to develop.
Factors Influencing Japanese Encephalitis Vaccine Cost
The cost of the Japanese Encephalitis vaccine can vary depending on several factors, including the manufacturer, country of administration, healthcare provider, and the number of doses required. Additionally, factors such as availability, demand, and government policies may influence the pricing as well. It's essential to research and compare the vaccine cost from different sources before making a decision.
Japanese Encephalitis Vaccine Cost Range
The cost of the Japanese Encephalitis vaccine can range from affordable to relatively higher, depending on various factors. It is advisable to consult healthcare providers, travel clinics, and vaccination centers to obtain accurate and up-to-date pricing information.
- Government Healthcare Programs: In some countries, the Japanese Encephalitis vaccine may be provided free of charge or at a subsidized cost as part of national immunization programs. Check with your local healthcare authorities or government health departments to determine if such programs are available.
- Private Healthcare Providers: Private clinics and hospitals may offer the Japanese Encephalitis vaccine at a cost that includes both the vaccine itself and any associated administration fees. The pricing may vary based on the specific provider and location.
- Travel Clinics: For individuals traveling to endemic areas, specialized travel clinics often offer comprehensive pre-travel healthcare services, including vaccinations. These clinics may have a separate pricing structure for Japanese Encephalitis vaccination, and it is recommended to inquire about the cost during the travel consultation.
Japanese Encephalitis Vaccine - Insurance Coverage and Reimbursement
In some cases, health insurance policies may cover the cost of the Japanese Encephalitis vaccine, either partially or in full. It is important to review your insurance policy or contact your insurance provider to determine the extent of coverage and any reimbursement options available.
Conclusion
Prevention of Japanese encephalitis is primarily achieved through vaccination. The Japanese encephalitis vaccine is recommended for individuals traveling to or residing in areas where the disease is prevalent. Travelers visiting or residing in areas with a risk of Japanese encephalitis are also advised to consider vaccination to reduce their chances of infection. If individuals experience symptoms, particularly neurological symptoms, it is crucial to seek immediate medical attention. Prompt medical evaluation is essential in such cases to ensure timely diagnosis and appropriate management.
Sources:
[World Health Organization (WHO) Japanese Encephalitis] (https://www.who.int/news-room/fact-sheets/detail/japanese-encephalitis)
[Centers for Disease Control and Prevention (CDC) Japanese Encephalitis] (https://www.cdc.gov/japaneseencephalitis/index.html)
https://ncvbdc.mohfw.gov.in/index1.php?lang=1&level=1&sublinkid=5773&lid=3693
https://nvbdcp.gov.in/Doc/JE-AES-Prevention-Control(NPPCJA).pdf
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6142657/
https://health.costhelper.com/japanese-encephalitis-vaccine.html
Medscape - Japanese Encephalitis (https://emedicine.medscape.com/article/233802-overview)
Ministry of Health and Family Welfare, Government of India (https://ncvbdc.mohfw.gov.in/index1.php?lang=1&level=1&sublinkid=5773&lid=3693)
https://www.medicalnewstoday.com/articles/181418
https://www.mayoclinic.org/drugs-supplements/japanese-encephalitis-virus-vaccine-intramuscular-route/description/drg-20072758
https://www.gov.uk/foreign-travel-advice
[Centers for Disease Control and Prevention (CDC) Japanese Encephalitis] (https://www.cdc.gov/japaneseencephalitis/index.html)
https://ncvbdc.mohfw.gov.in/index1.php?lang=1&level=1&sublinkid=5773&lid=3693
https://nvbdcp.gov.in/Doc/JE-AES-Prevention-Control(NPPCJA).pdf
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6142657/
https://health.costhelper.com/japanese-encephalitis-vaccine.html
Medscape - Japanese Encephalitis (https://emedicine.medscape.com/article/233802-overview)
Ministry of Health and Family Welfare, Government of India (https://ncvbdc.mohfw.gov.in/index1.php?lang=1&level=1&sublinkid=5773&lid=3693)
https://www.medicalnewstoday.com/articles/181418
https://www.mayoclinic.org/drugs-supplements/japanese-encephalitis-virus-vaccine-intramuscular-route/description/drg-20072758
https://www.gov.uk/foreign-travel-advice



 RSS Feed
RSS Feed